People often assume that all FDA-reviewed devices go through the same process. In reality, the U.S. Food and Drug Administration (FDA) uses multiple regulatory pathways, and the terms like FDA cleared, FDA approved, and FDA granted have specific meanings.
Understanding this distinction is important for healthcare professionals and patients, particularly in fast-moving fields such as neurology, digital health, and AI-enabled innovation.
Overview: Key Regulatory Pathways
At a high level, FDA clearance applies to most low-to-moderate-risk medical devices, while FDA approval applies to high-risk medical devices. A third pathway is De Novo, where the FDA “grants” a new device type for certain novel low-to-moderate risk devices with no predicate. These pathways differ significantly in risk classification, evidence requirements, review timelines, and cost. As a quick takeaway:
- FDA Cleared (510(k)): FDA determined the device is substantially equivalent to a legally marketed “predicate” device for its intended use.
- FDA Granted (De Novo): FDA classified a novel low-to-moderate risk device type when there is no suitable predicate.
- FDA Approved (PMA): FDA reviewed evidence intended to demonstrate a reasonable assurance of safety and effectiveness for many high-risk (Class III) devices.
- Exempt: Most low-risk (Class I) and some Class II devices do not require premarket review and can go directly to market, though they are subject to other controls.
People often say “FDA approved” as shorthand, but for many medical devices the more precise terms are cleared (510(k)) or granted (De Novo).
What Is FDA Approval?

FDA approval refers to the Premarket Approval (PMA) process, which is the FDA’s scientific and regulatory review to evaluate whether there is a reasonable assurance of safety and effectiveness for most Class III (highest-risk) devices.
This process requires manufacturers to provide independent scientific evidence, usually from extensive clinical trials, demonstrating a reasonable assurance that the device is safe and effective for its intended use.
The FDA provides an official overview of the PMA process on its website:
https://www.fda.gov/medical-devices/premarket-submissions/premarket-approval-pma
Key Characteristics of FDA Approval
FDA approval:
- Applies to life-sustaining or life-supporting devices
- Requires extensive clinical trials
- Involves a detailed review of safety and effectiveness
- Has longer timelines and significantly higher costs
- Often includes post-market study requirements
Examples of FDA-Approved Devices
- Implantable deep brain stimulation (DBS) systems
- Implantable neurostimulators used for epilepsy management and other neurological conditions
- Implantable continuous brain monitoring devices, such as long-term intracranial EEG systems used to detect and track seizure activity
These devices are typically implantable, life-sustaining, or life-altering, which places them in the FDA’s Class III (high-risk) category, requiring full FDA approval rather than clearance.
Example: A new implantable deep brain stimulation device for Parkinson’s disease must complete multi-year clinical trials and receive FDA approval via the PMA pathway before being marketed.
What Is FDA Clearance?

FDA clearance means a medical device has been reviewed through the 510(k) premarket notification process and found by the FDA to be substantially equivalent to an already legally marketed device. Such comparator devices are called predicate devices.
The FDA does not independently determine safety and effectiveness from scratch. Instead, it evaluates whether the new device is at least as safe and effective as an existing device already on the market.
The FDA provides an official overview of the 510(k) process on its website: https://www.fda.gov/medical-devices/premarket-submissions-selecting-and-preparing-correct-submission/premarket-notification-510k
Key Characteristics of FDA Clearance
FDA clearance:
- Applies primarily to Class II (moderate-risk) devices
- Requires comparison to a predicate device
- Typically relies on bench testing, software validation, and performance data
- Clinical trials are often not required
- Is faster and less expensive than FDA approval
Examples of FDA-Cleared Devices
Common FDA-cleared devices in the EEG and brain-monitoring industry include:
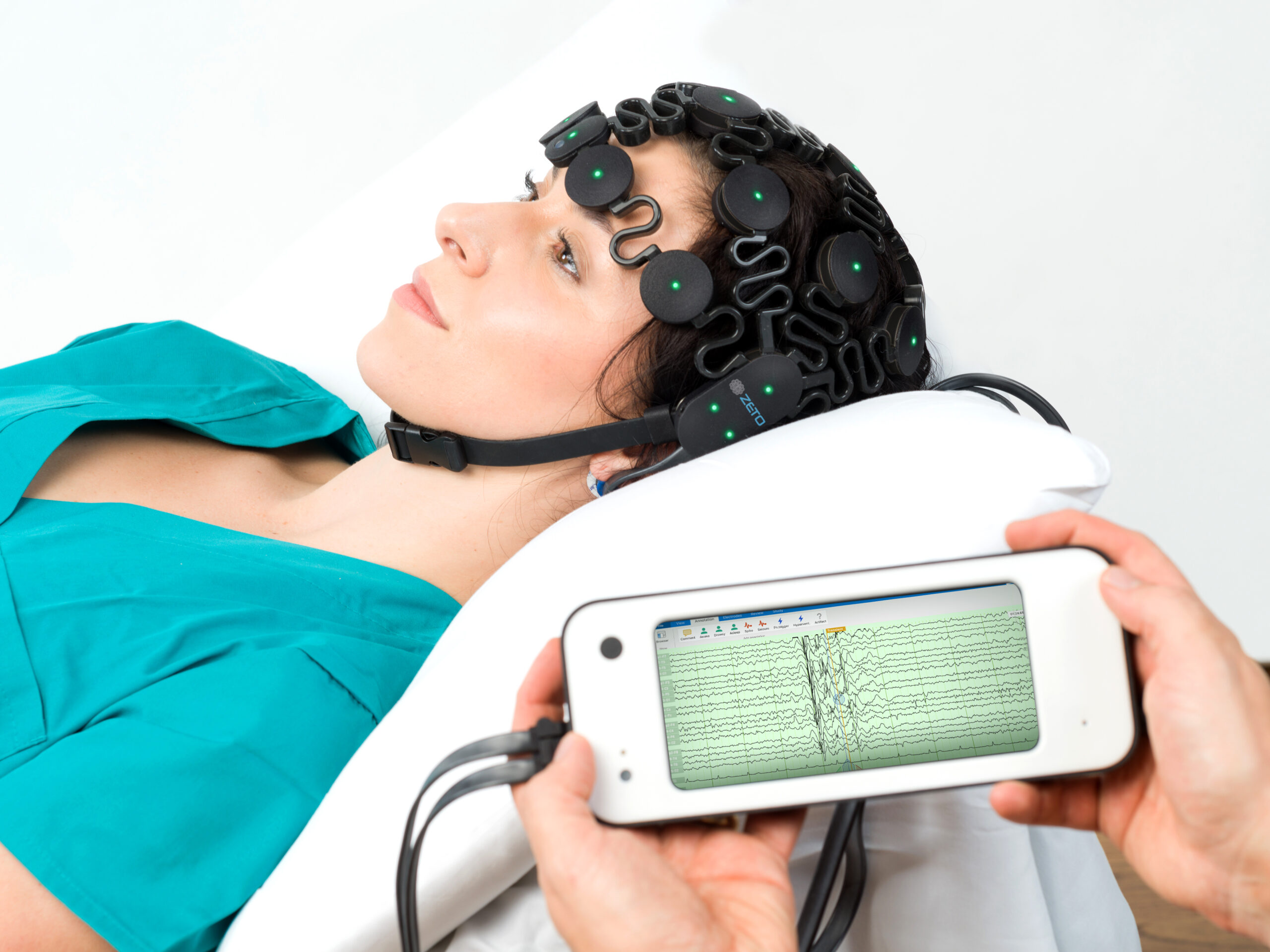
- Non-implantable EEG acquisition systems used in clinical, ambulatory, and point-of-care settings
- EEG analysis and visualization software, including cloud-based and AI-assisted interpretation tools
- EMG and evoked potential (EP) systems used for neurological diagnostics
- Neurophysiological patient monitoring systems for seizure detection and brain-state monitoring
- Wearable and portable brain-monitoring devices designed for remote, home, or outpatient use
These devices are typically classified as moderate-risk (Class II) and are cleared through the 510(k) pathway by demonstrating substantial equivalence to existing EEG and neurodiagnostic technologies already on the market.
Example:
A company develops a new EEG monitoring system that uses established signal-acquisition technology and has the same clinical indications as an existing EEG device. If it can demonstrate substantial equivalence to the existing device, it may receive FDA clearance through the 510(k) pathway.
What Is FDA “Granted” (De Novo)?

If there is no appropriate predicate device, a company may pursue the De Novo pathway for certain novel low-to-moderate risk devices. If granted, the FDA establishes a new device type, classifies it as Class I or Class II, and establishes any special controls required for Class II devices. Future devices of the same type can then use the 510(k) pathway.
Key Differences at a Glance
| Aspect | FDA Clearance | FDA Granted | FDA Approval |
| Regulatory Pathway | 510(k) Premarket Notification | De Novo | PMA |
| Risk Level | Moderate (Class II) | Low to Moderate (Class I & II) | High (Class III) |
| Predicate Device | Required | No | No |
| Clinical Trials | Often not required | Often Required | Required |
| Review Time | Months | Months | Years |
Common Misconceptions
“FDA cleared” does not mean “FDA approved.” These terms are not interchangeable, but both indicate the medical device can be legally marketed in the United States. Whether FDA cleared or approved, these devices’ manufacturers remain subject to quality system regulations, labeling requirements, post-market surveillance, and adverse event reporting.
An “FDA approved” label doesn’t inherently mean a device is better than an “FDA cleared” one. Those terms reflect FDA-defined regulatory pathways that are determined by a device’s risk classification, how well it fits within existing device types, and whether there’s an appropriate predicate, not a manufacturer’s preference for one label over another.
For many moderate-risk devices, the 510(k) pathway is available when a manufacturer can demonstrate the new device is substantially equivalent to a legally marketed predicate. In this pathway, the demonstration of substantial equivalence serves as a proxy for a direct demonstration of reasonable assurance of safety and effectiveness.
For example, an EEG system that can leverage a well-established, “gold standard” predicate may reach the market via 510(k) by demonstrating substantial equivalence to that predicate’s performance and intended use.
For PMA devices, showing similarity to a predicate is not considered sufficient evidence because the PMA standard is affirmative: the manufacturer must provide valid scientific evidence demonstrating a reasonable assurance that the device is safe and effective for its own specific intended use.
In higher-risk contexts, the FDA generally does not rely on substantial equivalence as a proxy for safety and effectiveness. Small differences in design, materials, software, human factors, or clinical workflow can meaningfully change the risk profile and clinical performance, and the consequences of unexpected failure are higher. As a result, the FDA typically requires direct evidence (bench, animal when relevant, and often clinical data) that addresses the device’s specific risks and demonstrates that the benefits outweigh those risks for the intended population and use.
Bottom line: ‘cleared’ versus ‘approved’ is about which regulatory route applies given FDA definitions and risk-based requirements. It is important to note that the fundamental legal standard for all pathways is to provide a reasonable assurance of safety and effectiveness; the pathway simply defines the method used to demonstrate it. The meaningful comparisons between devices come from their indications for use, claims, and supporting evidence, not from the cleared/approved label alone.
Final Thoughts
FDA clearance and FDA approval serve different but equally important roles in ensuring medical device safety in the United States. Clearance focuses on equivalence and performance for moderate-risk devices, while approval requires direct proof of safety and effectiveness for high-risk technologies.
For many innovations in neurology and digital health-especially those based on EEG technology-FDA clearance through the 510(k) pathway is the appropriate and established regulatory process, not a shortcut.
Disclaimer: This article is for informational purposes only and does not constitute legal or regulatory advice. The information provided is a general overview of FDA regulatory pathways and should not be relied upon as a substitute for consulting with a qualified regulatory professional. The FDA’s regulations and guidance are subject to change.