The Covid-19 pandemic has had negative effects on the health and well-being of many individuals around the world, often leaving persistent decreases in quality of life in the post-acute phase of illness. Studies of survivors across the globe, including the United Kingdom, Spain, the United States, and France found lasting neurological effects from Covid 19in thirty percent or more of study subjects when they were followed up after hospital discharge.¹
How does Covid 19 affect the brain?
In terms of how Covid 19 affects the brain, symptoms not only included fatigue and dyspnea, but also neuropsychiatric maladies, such as post-traumatic stress disorder (PTSD), anxiety, depression, and concentration and sleep abnormalities.¹ A prospective cohort study out of Wuhan, China showed similar results. Fatigue/muscular weakness (63%), followed by sleep disturbance (26%) and anxiety/depression (23%) were the most frequent lingering symptoms. Beyond effects on mood and energy, features of Covid-19 infection show that it can affect the brain and central nervous system, including loss of sense of smell and taste, concentration deficits, and headache.² At its most extreme, symptoms can include encephalopathy and seizure.

Source: Shutterstock
EEG Neurofeedback
EEG neurofeedback is a promising technique to provide clinical benefit to those suffering from neuropsychiatric complaints as an alternative or complementary therapeutic modality to conventional psychopharmacology, which carries the risk of many undesirable side effects.
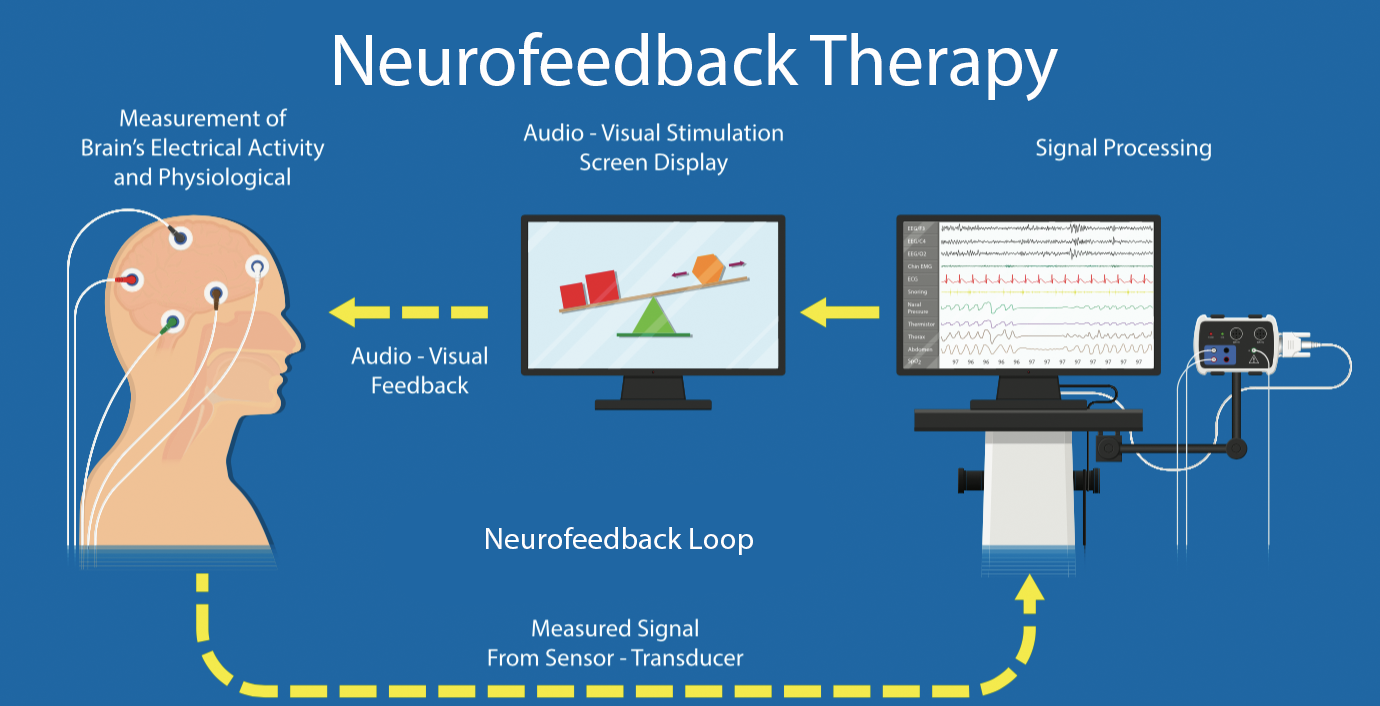
The International Society for Neuroregulation and Research explains the EEG neurofeedback process. They say, “During training, sensors are placed on the scalp and then connected to sensitive electronics and computer software that detect, amplify, and record specific brain activity. Resulting information is fed back to the trainee virtually instantaneously with the conceptual understanding that changes in the feedback signal indicate whether or not the trainee’s brain activity is within the designated range. Based on this feedback, various principles of learning, and practitioner guidance, changes in brain patterns occur and are associated with positive changes in physical, emotional, and cognitive states.”
A review article by Sharon Niv discusses this potential for a variety of disorders, including ADHD, autism spectrum disorders, substance use, PTSD, depression, sleep disturbance, and learning disabilities.³ Although most of these studies were not well-designed and placebo-controlled, the majority suggested clinical benefit.
A recent study by Ward, Porter, and Wood showed outpatient EEG neurofeedback reduced neuropsychiatric complaints, including hyperactivity, emotional lability, anxiety, and depression symptoms.4 Research by Escolano et al. demonstrated that neurofeedback could be effectively employed to enhance cognitive function (specifically working memory) that is negatively impacted by major depressive disorder (MDD).5 The benefit of neurofeedback in the setting of depression may be augmented by photic stimulation.6
Source: Shutterstock
EEG and Covid 19
An article by Kopańska et al. reviewed the most recent research on EEG findings in patients with COVID-19, including 17 publications in their evaluation.2 One pattern they identified was that changes frequently involved the frontal area of the brain, which controls focus and executive function. A nonspecific encephalopathic pattern was commonly found, although this pattern could be distinguished from infectious toxic encephalopathy or post-cardiorespiratory arrest encephalopathy using quantitative EEG (qEEG).7 Epileptic discharges and frank seizures or even status epilepticus were detected in a relatively small number of affected individuals.8 The degree of abnormality was associated with Covid severity and pre-existing neurologic disease.
Abnormal EEG patterns identified in patients with Covid-19 are potential targets for EEG neurofeedback. Luckos, Cielebak, and Kaminski published a case study on the therapeutic potential of this modality specifically for Covid.9 A 48-year-old woman developed neurocognitive deficits described as “brain fog” about a month after contracting Covid-19 infection. Her decline was so severe that she was no longer able to function independently.
EEG neurofeedback coupled with goal-directed cognitive training behavioral training was able to greatly alleviate her symptoms, and she was able to resume work. Others affected by Covid’s lasting neurological effects might similarly benefit.
It seems clear that Covid 19 impacts the brain, and that Covid causes lasting neurological effects. It seems equally clear that EEG neurofeedback may be a big help to those who have had Covid 19.
References
1. Nalbandian A, Sehgal K, Gupta A, Madhavan MV, McGroder C, Stevens JS, Cook JR, Nordvig AS, Shalev D, Sehrawat TS, Ahluwalia N. Post-acute COVID-19 syndrome. Nature medicine. 2021 Apr;27(4):601-15.
2. Kopańska M, Banaś-Ząbczyk A, Łagowska A, Kuduk B, Szczygielski J. Changes in EEG recordings in COVID-19 patients as a basis for more accurate QEEG diagnostics and EEG neurofeedback therapy: a systematic review. Journal of clinical medicine. 2021 Jan;10(6):1300.
3. Niv S. Clinical efficacy and potential mechanisms of neurofeedback. Personality and Individual Differences. 2013 Apr 1;54(6):676-86.
4. Ward KP, Porter NA, Wood DS. The effectiveness of neurofeedback in an outpatient setting: A multilevel modeling approach. Research on Social Work Practice. 2019 Nov;29(8):939-48.
5. Escolano C, Navarro-Gil M, Garcia-Campayo J, Congedo M, De Ridder D, Minguez J. A controlled study on the cognitive effect of alpha neurofeedback training in patients with major depressive disorder. Frontiers in behavioral neuroscience. 2014 Sep 2;8:296.
6. Hammond DC. Neurofeedback treatment of depression with the Roshi. Journal of Neurotherapy. 2000 Jun 1;4(2):45-56.
7. Pastor J, Vega-Zelaya L, Martin Abad E. Specific EEG encephalopathy pattern in SARS-CoV-2 patients. Journal of Clinical Medicine. 2020 May;9(5):1545.
8. Antony AR, Haneef Z. Systematic review of EEG findings in 617 patients diagnosed with COVID-19. Seizure. 2020 Dec 1;83:234-41.
9. Luckos M, Cielebak K, Kaminski P. EEG NEUROFEEDBACK IN THE TREATMENT OF COGNITIVE DYSFUNCTIONS AFTER THE INFECTION OF SARS-CoV-2 AND LONG COVID-19. Acta Neuropsychologica. 2021:361-72.